Dr. Eckland Answers Shoulder Replacement Questions
Considering joint replacement is a big decision, we want our patients to be as informed as possible about the process and what to expect before making the final call. Dr. Chris Eckland, a sports medicine physician at Sano Orthopedics, reviews some important information about shoulder replacements.
What is a shoulder replacement?
A shoulder replacement, or shoulder arthroplasty, is a procedure that tries to eliminate the source of pain and dysfunction by replacing damaged parts of the shoulder joint with artificial components. The artificial joint, which is also called a prosthesis, is designed to move like a regular, healthy joint so your shoulder can function normally again.
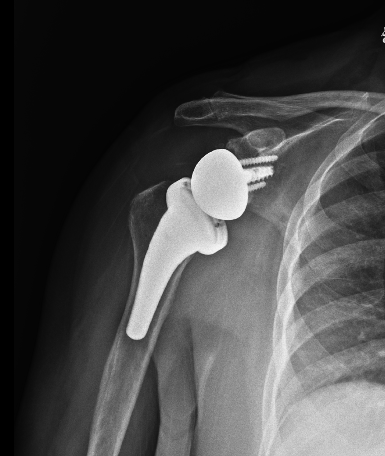
When is it time to consider a shoulder replacement?
Many different conditions could lead to a person requiring shoulder replacement. The most common reasons for a shoulder replacement surgery include:
- Osteoarthritis – This degenerative condition causes stiffness and pain in the shoulder joint and is the most common reason for shoulder replacement.
- Rotator cuff tear arthropathy – Long-term rotator cuff tears left unaddressed can sometimes lead to arthritis. Joint replacement may be the best option for restoring function.
- Avascular necrosis – the death of bone from loss of blood supply (long term steroids, excess alcohol, post-traumatic, sickle cell disease, and other blood disorders etc.)
- Shoulder fracture – Joint replacement sometimes becomes the best option to replace a broken bone, stabilize the joint and restore function.
The procedure is meant to relieve your pain, improve your strength, increase your range of motion and enable you to use your shoulder and arm.

What is the recovery like after shoulder replacement?
As with every surgical procedure, the recovery time is patient-centered. Shoulder replacement recovery varies based on multiple factors. These factors include age, shoulder disease, medical comorbidities, weight, activity level, general pain tolerance, and more importantly, adherence to postoperative instructions and physical therapy protocols. Physical therapy is crucial to a successful outcome!
Key recovery phases:
Phase 1: Sling immobilization for 2-6 weeks. During this phase, there is limited movement. This means patients must limit lifting and avoid strenuous activities. Work will be allowable at this time with limitations of motion.
Phase 2 (4-8 weeks): Progress from passive range of motion to active range of motion with physical therapy. The sling is discontinued, but lifting and activity are still limited.
Phase 3 (6-12 weeks): This is where we began progressive strengthening. Some lifting restrictions are lifted.
Phase 4 (12- 20 weeks): Continue progressive strengthening and return to full activity between 12 and 20 weeks depending on surgical type is and medical status.
Complete recovery typically does take a full year. Although strength will continue to increase as well as coordination up to 2 years postop.
What are the different types of shoulder replacement?
- Anatomic total shoulder replacement. Both the ball and the socket are replaced. The implants resemble the natural shape of the bones.
- Reverse total shoulder replacement. Both the ball and the socket are replaced, but the implants are reversed. The ball is attached to the shoulder blade and the socket is attached to the upper arm bone. This option typically is preferred if the rotator cuff is severely damaged.
- Partial shoulder replacement. Only the head (ball) of the joint is replaced. It may be recommended when only the ball side of the joint is damaged.
Is shoulder replacement right for me?
Shoulder replacement surgery should be a collective decision between you and your physician. Shoulder replacement decision considers the patient’s well-being and goals.
Shoulder Replacement: Keys to a Successful Recovery
- Do not focus on the day, rather focus on hitting milestones and goals. It is a long process that requires commitment for the best results.
- Nobody is a “fast healer.” Healing rates are based on biology which is very predictable in most cases.
- It is important to trust your surgeon. If you don’t, seek a second opinion. It will increase your comfort level with the process. You must be able to voice your concerns if you feel something is wrong. Early intervention or change in strategy is always easier than dealing with a lingering problem.
- Have trust in the recovery protocol with regards to physical therapy and restrictions. It is important to remember that the surgeon has nothing to gain by restricting any longer than you need to be. This is an effort to avoid complications and keep the recovery on the appropriate timeline.
Common Shoulder Replacement FAQs
How long does the surgery take to perform?
Surgery does vary based on her degree of shoulder dysfunction, but the typical time frame is 45-90 minutes of surgical time.
How long will I be in the hospital?
Most patients can go home the same day. however, based on some medical issues as well as other factors like age, some patients may require an overnight stay.
What are the risks with shoulder replacement?
As with any surgery, there are inherent risks for complications. These risks are relatively low but adherence to the recommendations of your surgeon, and physical therapist following surgery, significantly decrease the risk of complication. Risks include: dislocation, fracture, rotator cuff injury, infection, injury to nerve or blood vessel, stiffness, implant loosening, blood clot.
Meet Dr. Chris Eckland
Orthopedic Sports Medicine Surgeon
Dr. Chris Eckland is a fellowship-trained and board-certified orthopedic surgeon specializing in shoulder, sports medicine, knee, and fracture care. He has a special interest in shoulder joint replacement.
“Once a patient decides to proceed with shoulder replacement recovery can be somewhat daunting and timely. I often tell patients that only 10-20% of their outcomes are based on the surgery itself and the rest is based on the success of recovery. One common point that typically occurs is within 1-2 weeks patient realizes that the pain after surgery is significantly different than the pain before surgery and likely represents postsurgical pain. This often motivates patients because they realize the surgery achieved the intended purpose.” – Dr. Eckland

